Is community mask-wearing effective in reducing the spread of SARS-CoV-2? Numerous observational, epidemiology, laboratory, and modeling studies have suggested that masks work. The results of these studies are now supported by the first massive randomized controlled trial, the gold standard in medical research, conducted in the real world. In this post, one of the principal investigators of this new randomized controlled study, Laura Kwong, PhD (Assistant Professor of Environmental Health Sciences, University of California, Berkeley), shared her insights about the study in an interview with Maker Mask and India Covid SOS.
Introduction
Researchers at Stanford and Yale partnered with Innovations for Poverty Action in a large-scale randomized controlled trial on mask interventions and their effects on symptomatic SARS-CoV-2 infections in rural Bangladesh. This study provides strong real-world evidence that mask wearing, particularly surgical mask wearing*, is effective in reducing symptomatic SARS-CoV-2 infections. The study also shows that targeted and scalable interventions to promote mask-wearing can increase mask use.
- [Update December 2, 2021] This study is now published and can be found here.
- A more lay person-friendly overview of the study penned by one of the principal investigators of the study is available here.
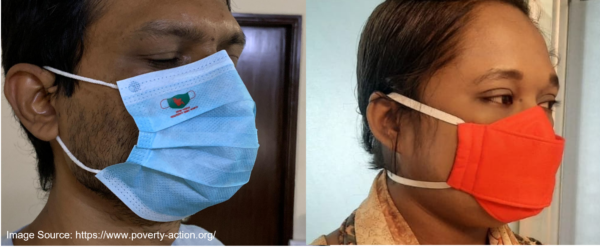
* TerminologyIn this post, the terms “surgical mask” and “cloth mask” refer to specific masks defined in the study and should not be generalized to be inclusive of all surgical masks or all cloth masks. Other studies have demonstrated that mask performance varies significantly within these broad categories. The following are the specifications for the two types of masks used in this study (Figure 1):
** Surgical masks are generally considered disposable (single-use) and should not be washed and reused. However, the investigators of the Bangladesh Study tested the specific masks used in this study with their washing protocol and determined filtration after washing remained sufficient to warrant their continued use (details are slated for a future publication). In general MakerMask does not recommend washing and reusing surgical masks without express instructions and testing data from the manufacturer (e.g., compliance with the ASTM F3502 standard for reuse) |
Questions and Answers with Dr. Laura Kwong
Could you please give us an overview of this study?
We conducted a cluster-randomized trial of community-level mask promotion in rural Bangladesh from November 2020 to April 2021. We involved 600 villages. That’s over 350,000 adults in rural Bangladesh. In 300 villages, we did not encourage masking, but of course people were able to wear masks as they had been doing before. In another 300 villages, we promoted mask wearing–in 200 villages, we used surgical masks for that promotion; and in 100 villages, we used cloth masks.
For the promotion, our team distributed free masks to households. We provided information that Covid could be in rural villages, and that mask could be helpful to prevent Covid. We showed a movie of respected people–including the prime minister, the head of the national imam training academy, and a national cricket star–talking about the importance of wearing masks, and encouraging people to wear masks. We had role modeling by political and community leaders wearing masks, and also encouraging people to wear a mask at Friday Jum’ah prayers. In addition, we had community-wide in-person reinforcement, to remind people to put on the mask they received (from household distribution), or to give them a new mask. We did the intervention for eight weeks and we asked about symptoms of Covid. We collected blood from symptomatic people and we tested that for Covid antibodies to see who actually had been infected. The primary outcome was symptomatic infection with SARS-CoV-2. The secondary outcome was mask wearing.
The study reported that in villages with mask interventions, there were fewer cases of symptomatic COVID-19 cases. Can we conclude from this study that masks are effective in reducing symptomatic infection with SARS-CoV-2 (aka COVID-19)?
Yes. Mask wearing in the control villages was 13%. Mask wearing in the intervention villages was 42%. So we saw a 29% increase in mask wearing in intervention villages compared to the control villages, and this resulted in a 9% reduction in Covid.
In villages with surgical mask intervention, we saw an 11% reduction in Covid. We also considered how the impact of our surgical mask intervention differed between subgroups. With people over 60 years old, we saw a 35% reduction in Covid. For people 50 to 60 years old, it was a 23% reduction. So we have really solid evidence that surgical masks are effective in reducing Covid.
Are the results statistically significant?
For surgical masks, the reduction in Covid rates for the intervention villages was statistically significant. For cloth masks, we find a statistically non-significant 5% reduction in Covid cases. However, both mask types, surgical and cloth, reduced Covid-like symptoms by 12%, and this was statistically significant for both surgical and cloth masks.
Even in villages with intervention, you observed <50% mask adoption. What are some barriers for mask adoption? Do you have recommendations on how to further increase mask adoption rates? How would that affect COVID-19 transmission?
We increased mask-wearing substantially, but in the end, we only got to about 45% mask adoption. Mask adoption started out very low, around 15%. It’s really important that you noticed that because we likely could have seen much larger impacts had there been more mask-wearing.
Let’s assume we started at 50% mask adoption instead. Assume that our intervention still resulted in a 29% increase–this would get us up to 79% mask adoption. We expect a non-linear impact of masking in the same way that we would expect a non-linear impact from vaccine coverage: because it’s a network effect, the impact scales faster with more participants. So if there was a higher level of mask adoption, the effects on Covid reduction would have been much stronger. Our finding that increased masking reduced Covid by 9% is probably a lower bound on the effect of masks given the low mask adoption that we started with.
We’re conducting focus group discussions right now to better understand why people didn’t wear masks. One reason could be that people still didn’t see the need. Rural Bangladesh is a largely outdoor society. People are working in the fields; markets are outside and uncovered. People may not perceive that they really need to wear a mask.
This study is focused on rural uptake of masks in Bangladesh, with an observed population that is 88.2% male. Which parts of the study would you expect to be applicable in different cultural contexts such as the U.S., and which parts do you think wouldn’t translate well to other cultural contexts?
Promoting masks is very different in politicized regions and non-politicized regions. In politicized regions, we think that role modeling by individuals can be very effective, if it comes from a politically aligned figure.
In our study in Bangladesh, we didn’t use mandates to increase mask-wearing. Our message was that we’re giving you a mask and we care about you. We politely reminded people to wear their masks, and gave out another mask if they forgot theirs. We made mask wearing very convenient–with people demonstrating mask wearing, and with plenty of masks available. We did two rounds of piloting before we conducted the large-scale study; the first round of piloting did not include in-person reinforcement while the second round did. We found substantially higher uptake in the round that involved in-person reinforcement, suggesting that social pressure generated by in-person reinforcement is a valuable part of our intervention.
As detailed in the paper, we tried a number of other incentives and behavior change strategies. We sent text messages with reminders. We used both altruistic and self-protection language. We tried incentives, both monetary incentives and non-monetary. We had people post a sign on their door declaring it as a mask-wearing household, or make verbal commitment to mask wearing. Many of these strategies didn’t work, but it could be specific to our particular setting
In rural societies in South Asia, particularly Muslim societies, it is common to have mainly men out and about. I don’t think we would necessarily promote masks differently if we had more women, except we would probably have more female promoters, or we would target areas where more women congregate–for example, community centers, or the women’s section in the local mosque.
Could you please tell us more about the masks used in this study? How many masks were issued? What were the cleaning instructions?
Both types of masks were made locally in Bangladesh.
Surgical Mask Details: The surgical mask had three layers of 100% non-woven polypropylene (the exterior and interiors were spunbond and the middle layer was meltblown), elastic ear loops, and a nose bridge, with a filtration efficiency of 85% to 95% with 0.3 um particles. We put a sticker on the surgical mask signifying that it could be washed and reused. The instructions for washing were to wash when the mask was visibly dirty or smelly. Wash with either powder detergent or with a bar of soap. Put the mask between your hands and rub gently. Rinse it out in running water, then squeeze out (not wring) excess water. Hang dry.
As expected, the surgical mask showed a decrease in the filtration efficiency after washing due to the loss of electrostatic filtration effects. But even after washing, the filtration of our particular surgical mask was still substantially higher than our cloth mask. We will have another paper that goes into more details on the filtration efficiency of these masks that were used and washed in the real world.
Cloth Mask Details: The cloth mask had an exterior layer of 100% non-woven polypropylene (70 grams/square meter [gsm]), two interior layers of 60% cotton / 40% polyester interlocking knit (190 gsm), an elastic loop that goes around the head above and below the ears, and a nose bridge. These materials were chosen because we found them to be effective, and they could be locally sourced. The cloth mask was made in a 3D/boat shape style, the same style that’s used for KF94s. The filtration efficiency was 37%, and no filtration degradation was observed after washing (same washing instructions as the surgical masks). Note that the initial filtration efficiency of our cloth mask is significantly lower than our surgical mask.
For the cloth mask design, people liked the head straps because –they were easy to adjust to the face and the mask could hang around the neck when not in use. We cobbled things together from all the work that the mask community has done. We really do appreciate the many attempts and trials that people have been doing for months. Thank you mask community!
Within the eight-week intervention period, we gave out approximately 6 cloth masks per person, and 8 surgical masks per person. This is more cloth masks than you might think if everyone was truly reusing their cloth masks all the time. But we did not want to stymie ourselves by having a limited supply of masks, so we did everything we could to make sure people had masks, even if it meant giving out additional masks when they forgot theirs at home.
The study split mask intervention villages into two groups–⅓ of the intervention villages got cloth masks, and ⅔ of the intervention villages got surgical masks. Why didn’t you split the groups equally?
Cloth masks were really expensive. The cloth masks in our study were 40 cents each. The surgical masks were 6 cents each, with an additional 7 cents for our sticker (for a total of 13 cents each). By using the cheaper surgical masks, we could afford to enroll more villages. So it wasn’t an even split because of the cost.
In comparison to control villages with no intervention, the study reported that villages with surgical mask intervention showed a statistically significant reduction in symptomatic SARS-CoV-2 infections, whereas villages with cloth mask intervention showed a modest or no reduction in symptomatic SARS-CoV-2 infections. What is the proper way to interpret this result? Does the fact that there are roughly twice as many people in the surgical mask group than in the cloth mask group affect the statistical significance of the cloth masks vs. surgical masks results?
Our study was not designed to compare the impact of surgical masks on Covid compared to the impact of cloth masks on Covid. Instead we compared the impact of any proper mask-wearing on Covid. If we had wanted to compare the impact of surgical vs. cloth, we would have required a much larger sample size and we would have had an equal number of cloth and surgical villages to improve the statistical power of the comparison. Due to cost factors, we did not split the surgical and cloth mask villages evenly, using twice as many surgical masks as cloth. We did not identify a statistically significant difference when we compared the results in the surgical mask village to the results in the cloth mask village because our study was not powered to compare surgical and cloth masks. Further study is needed for that comparison.
Based on our results, we are advocating for surgical masks when the choice is available, because we saw the strongest evidence that they are effective in reducing symptomatic SARS-CoV-2 infections.
The use of cloth masks and the use of surgical masks both significantly reduce Covid-like symptoms. This tells us that using a mask of any kind is helpful to reduce the burden on health.
Based on this study, would you recommend people to upgrade to higher filtration masks?
Yes, I think everybody should be wearing higher filtration masks. Although our study was not powered to compare surgical masks against cloth masks, nor did we identify a statistically significant difference when we attempted to compare them, our hypothesis is that a mask with better filtration can better reduce Covid transmission.
Note that the terms “surgical mask” and “cloth mask” in the paper are specific to the masks we used. Those terms are not generalization of all surgical masks or all cloth masks. There are low quality surgical masks that only filter at 30%–they’re 2-ply, and they are surgical masks, but they are not the same quality as the ones we used in the study. Similarly, some hybrid masks (cloth masks with filters or specialized materials that are not commonly available) feature high filtration materials. It is beyond the scope of our paper to address the varieties of masks out there.
I recommend high quality surgical masks, KF94s, KN95s, or N95s. The trick with KN95s right now is that a lot of them are counterfeit, according to CDC data. So I think you have to be careful when purchasing a KN95. Buy only from reputable sources. This document is a great resource on high-performance masks.
What are some of your plans for future studies?
We are doing a follow-on study in the same locations in Bangladesh to look at the effect of higher filtration masks against the Delta variant. We’ll be looking at asymptomatic infection as well as symptomatic infection. We’ll be using KF94s and surgical masks. We chose surgical masks because they’re cheap, allowing us to include more villages. We chose KF94s because they’re good quality masks with high filtration, and a bit more comfortable in some ways. Some people might also think they look less funny than KN95s, as KF94s actually have the same boat shape as the cloth mask we used before.
However, currently KF94s are basically non-existent in the market in South Asia. For the study, we will likely import them directly from Korea or China. We have talked to our local manufacturers who made the surgical masks. They are open to the idea of purchasing the supplies for the KF94 manufacturing process and making them in Bangladesh, if that proves to be reasonable from a business standpoint. Our hope is that eventually more countries can produce KF94-like masks and follow similar regulatory systems as Korea. Korea is one of the few countries that has manufacturing guidelines and standards for a public-use mask.
We’re currently doing focus discussions with rural Bangladesh community members to assess what they think about the different types of masks–surgical, cloth, KN95, and KF94. Which ones would they be willing to wear? How far do we promote and push for the importance of balancing fit, filtration, and breathability? Many people in rural areas are agricultural. They’re doing manual labor and breathability is very important. KF94 is a better mask than a surgical mask, because it has a higher filtration and a better fit. But for some, they may find a KF94 too snug and uncomfortable, and they are just not going to wear it. So perhaps in some cases, it’s better to have a surgical mask with slightly worse fit (more leakage), if more people are willing to wear it because they feel it is easier to breathe. Based on the results of these discussions, we will come up with a plan on how to address people’s concerns.
We’re also working with a behavioral psychologist to come up with other strategies that might increase mask wearing. We will be doing pilot studies before a large scale rollout.
In the US, we are hoping to reach out to more reticent populations, to think about how to increase mask wearing. In Sub-Saharan Africa, we are pursuing work with a group that works with different religious faith leaders to leverage their community ties.
Sustainability is one of the concerns in adoption of disposable masks. What are your thoughts on this, as you promote disposable high performance masks?
In our study, we reduced waste by using high quality surgical masks that can be washed and reused. We’re currently working on a lab-based study to understand how washing affects breathability and filtration efficiency and exactly how many times different types of surgical masks can be washed and reused.
Looking at the overall cost/benefit analysis–there are many other things that are producing environmental waste and pollution. We can definitely do better to have environmental standards that prevent pollution, so it’s still waste, but it’s not pollution. Bangladesh did a study in the first month of their lockdown and they found that plastic bags used for carrying food produced three times as much plastic waste as surgical masks, even though plastic bags were banned in Bangladesh! To put things in perspective: Plastic bags cause waste and pollution, and cannot save lives. Disposable masks cause waste, but they can also save lives!
Note: This interview has been edited for length and clarity.


